ICU Beds: Key Features, Specifications & Differences from Other Hospital Beds
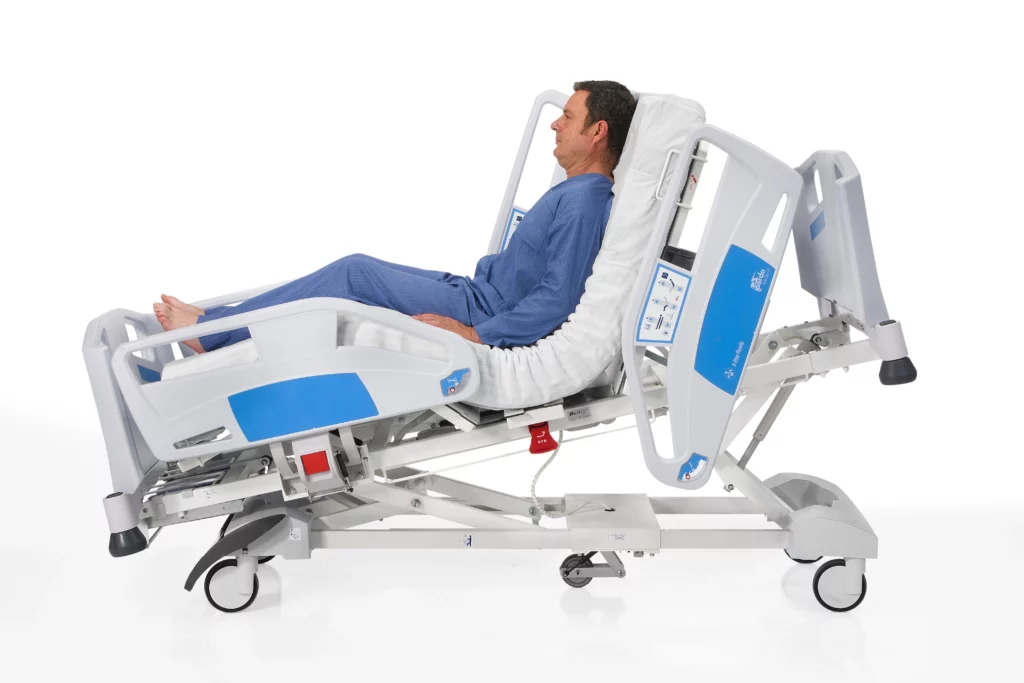
Intensive care units (ICUs), also known as critical care units (CCUs) or intensive therapy units (ITUs), provide life-saving care to patients who are seriously ill or critically injured. In these environments, ICU beds play a vital role, offering specialized functions that support both patient care and medical staff efficiency. But how do ICU beds differ from standard hospital beds used in general wards? This article will explore the specifications, features, and differences that make ICU beds essential for critical care settings.
ICU Bed Specifications
ICU beds are not just a type of bed—they’re purpose-built for intensive care units. While any bed used in an ICU can technically be called an ICU bed, there are specific guidelines and features that distinguish them from beds used on general hospital wards.
Department of Health and Social Care Guidelines
According to the Critical Care Unit Planning & Design Notes from the Department of Health and Social Care, each ICU bed should meet three key specifications:
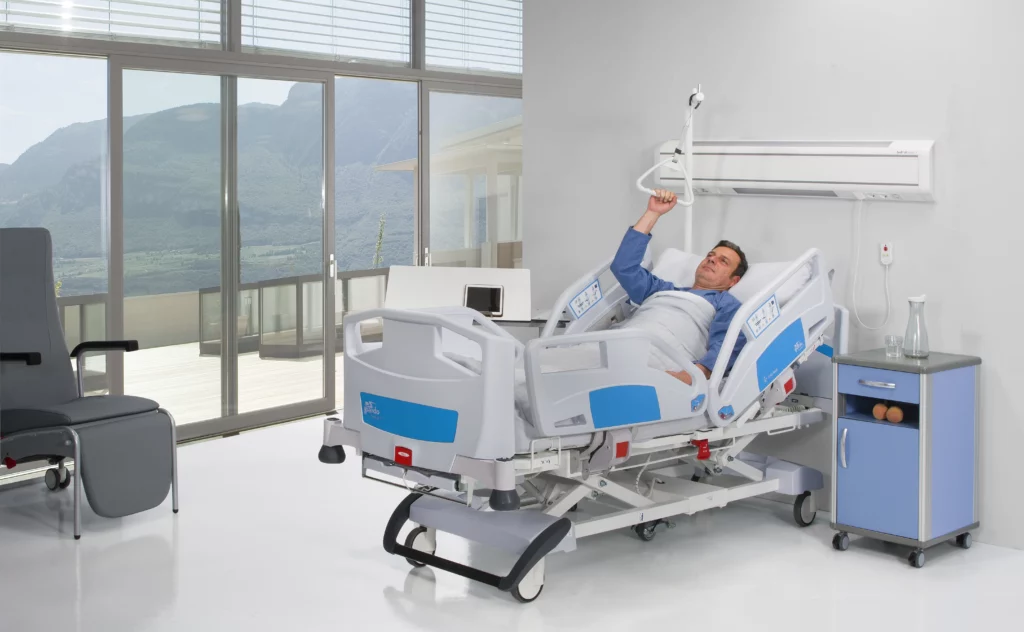
- Electric Operation: ICU beds must be electric, allowing staff to adjust the bed’s position via a handset or control panel. This eliminates the need for manual adjustments, saving time and ensuring safety for both patients and staff.
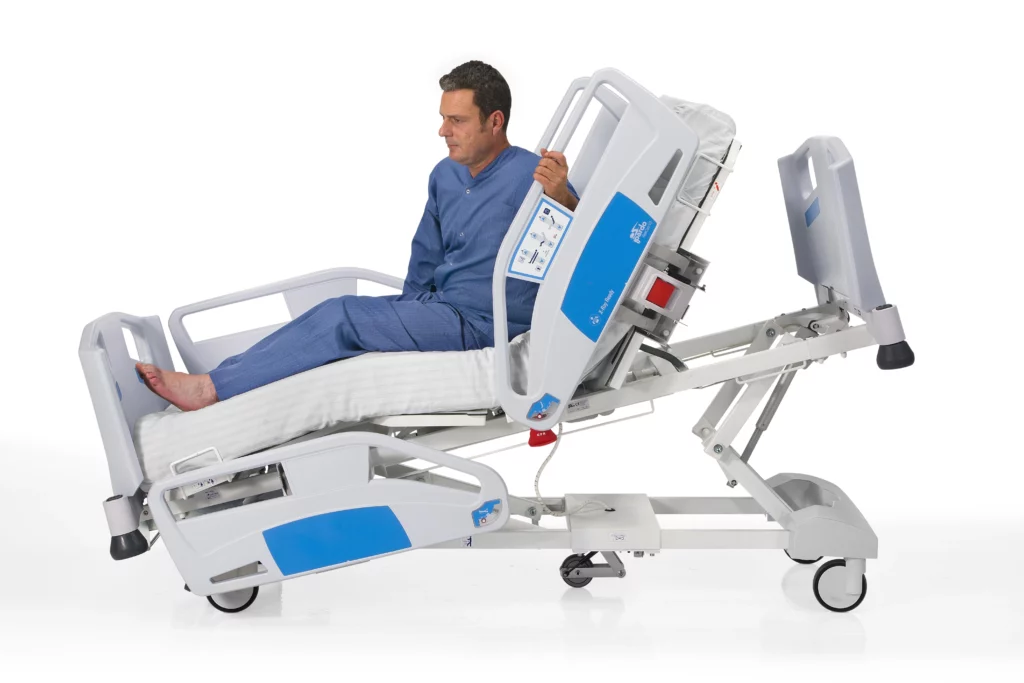
- Cardiac Chair and Trendelenburg Positioning: These functions help optimize patient respiration and circulation, both critical for ICU patients.
- Pressure-Relieving Mattress: ICU beds are designed to accommodate pressure-relieving mattresses, which help prevent pressure ulcers and ensure patient comfort.
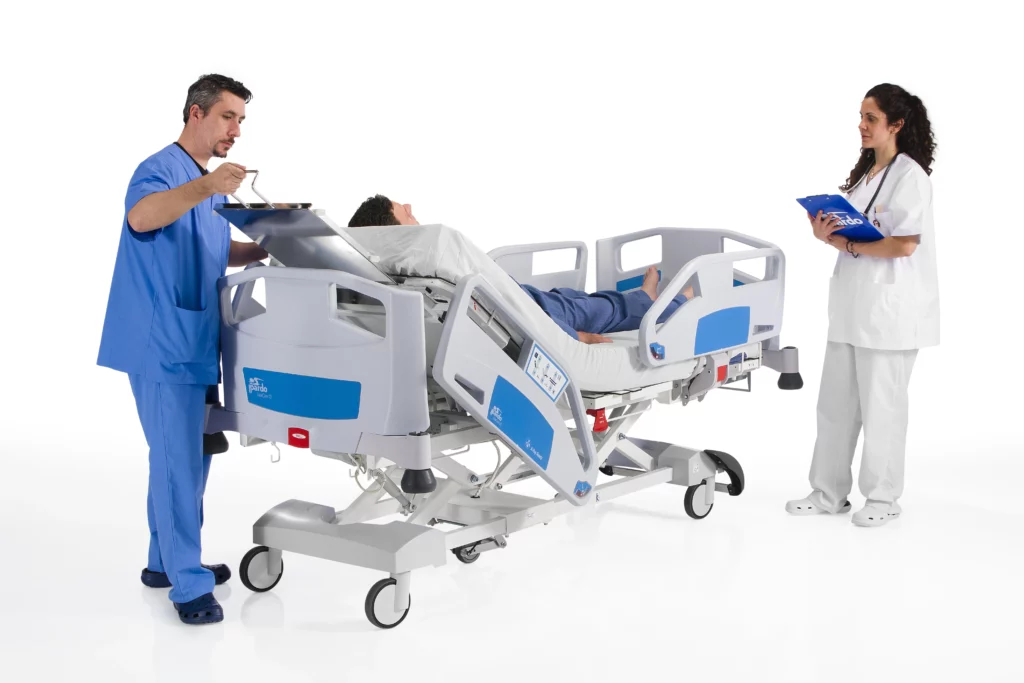
4 Essential Features of ICU Beds
When it comes to ICU beds, functionality is key. These beds are equipped with several important features that are essential for critical care settings:
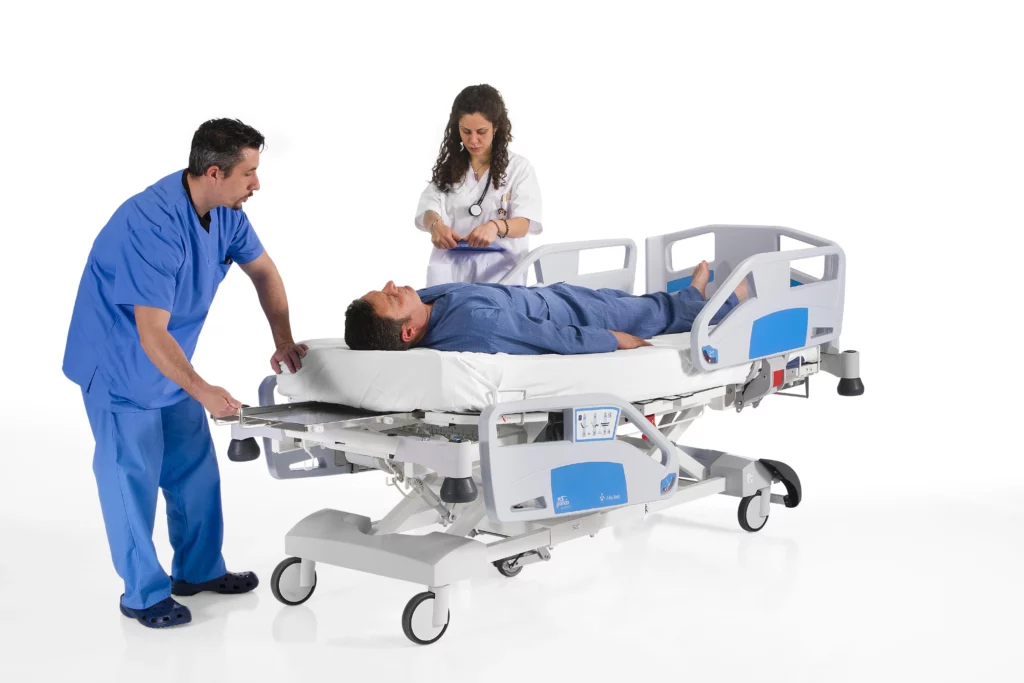
1. CPR Release Function
In emergency situations, the CPR release function allows the bed to be quickly flattened, providing a firm surface needed for performing CPR. This feature can be activated at the push of a button or lever, allowing staff to respond rapidly during emergencies.
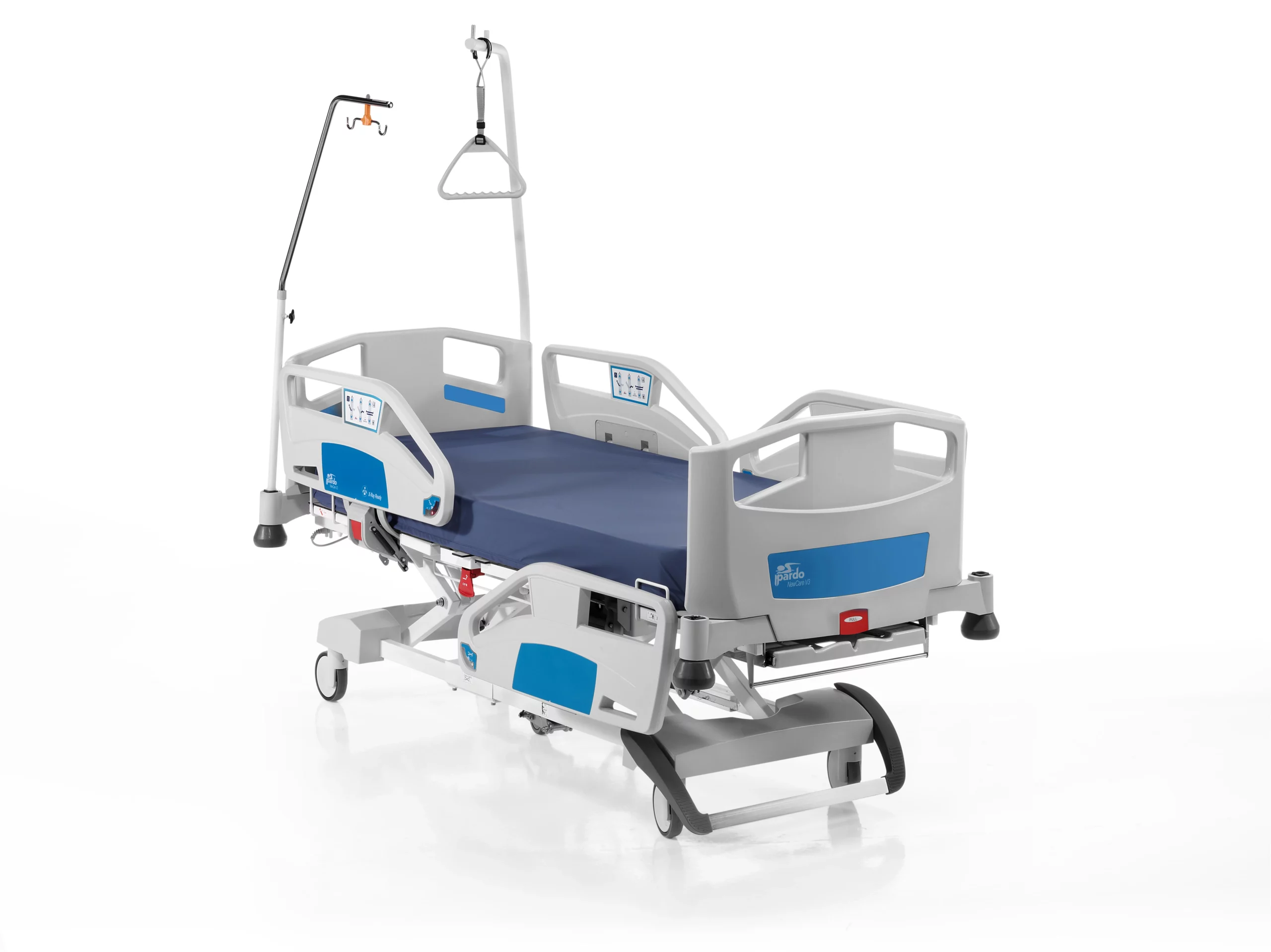
2. IV Poles with Multiple Hooks
ICU beds typically come with IV poles that have multiple hooks for hanging medications or fluids. This is especially useful in critical care situations where patients may require multiple drips or infusions simultaneously. The inclusion of IV poles on the bed simplifies the movement of patients, ensuring everything is moved together in case of an emergency.
3. Removable Head and Footboards
Beds with removable head and footboards are often preferred in ICUs because they provide more flexibility during emergencies. Removing the headboard allows medical staff better access to the patient’s head for resuscitation or other critical interventions. It also aids in performing procedures like prone positioning, which is shown to improve respiratory function in critically ill patients.
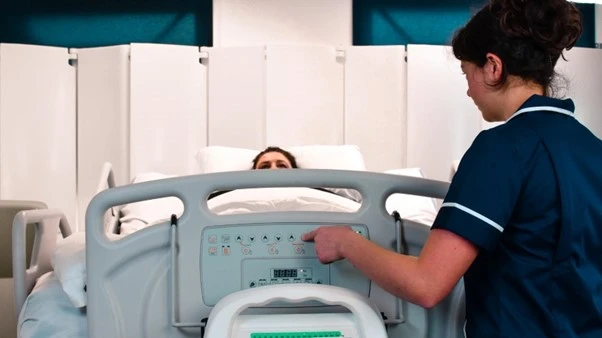
4. Nurse Controls
Many ICU beds come equipped with nurse control panels that allow staff to adjust bed functions without relying on the patient’s handset. This is especially useful for locking certain functions to prevent patient accidents or injuries. Nurse controls also reduce the risk of tripping over wires and ensure quick, immediate access to bed adjustments when time is of the essence.
ICU Beds vs. General Hospital Ward Beds
While both ICU beds and general hospital ward beds serve the purpose of patient care, the design and features of ICU beds are far more specialized to meet the demands of critical care.
Levels of Care in Hospitals
In the UK, hospital patients are classified based on their care needs, ranging from Level 0 (normal ward care) to Level 3 (advanced respiratory support and multi-organ system support). ICU beds are primarily used for patients in Level 2 and Level 3 care, who require intensive monitoring and intervention. The features of ICU beds, such as CPR release and adjustable positioning, are crucial for meeting these higher levels of care, where rapid response and precise patient positioning can make a life-saving difference.
Supporting Critical Care in Emergencies
ICU beds are designed for quick interventions and continuous monitoring, which is vital when treating patients with complex conditions. In contrast, general hospital ward beds, while still equipped with essential functions, do not typically have the same features that facilitate fast medical responses. For example, standard beds may not offer adjustable positions or accommodate specialized mattresses like those in ICU beds.
Flexibility: ICU Beds Beyond the ICU
While ICU beds are primarily used in intensive care units, many hospitals also place them in other areas where high-dependency care is required. For instance, during emergencies or sudden patient surges, ICU beds can be used in recovery rooms, surgical areas, or even in hospital wards temporarily transformed into critical care spaces. The versatility of ICU beds makes them an essential asset in any hospital’s arsenal, ensuring that hospitals are prepared for any emergency, especially during times of increased patient demand.
Conclusion
ICU beds are far more specialized than standard hospital beds, providing crucial features that support patient care and enable rapid medical interventions. From electric adjustability to CPR release functions, ICU beds are built to handle the complexities of critical care. As healthcare settings continue to evolve, these beds remain integral to delivering high-quality, responsive care to patients in intensive care units and beyond.
Interested in learning more about ICU beds or need support sourcing them for your hospital? Get in touch with our team at Innova to explore our range of ICU beds and other specialized healthcare solutions.